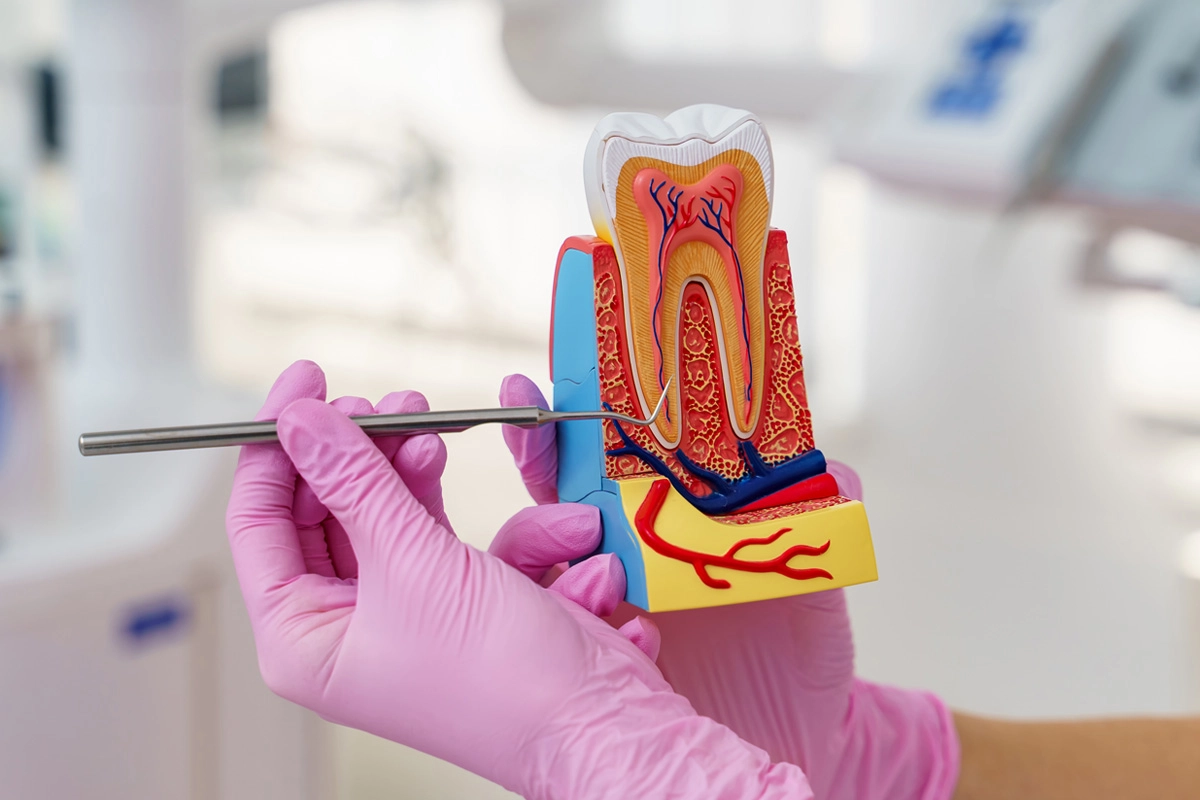
What is root canal treatment?
Root canal treatment is a treatment method applied in cases where the pulp, which is a soft layer consisting of a vascular-nerve bundle in the innermost part of the tooth, is damaged in such a way that it cannot repair itself.
This treatment involves the removal of the crown and root pulp, usually under anaesthesia, mechanical enlargement of the root canals to free them from microorganisms, and then sealing them with a special filling material up to the root tip.
What happens if root canal treatment is not performed?
If inflamed or damaged pulp is not removed, it can cause infection in the tooth and surrounding tissues and lead to tooth loss.
What are the conditions that require root canal treatment?
The main conditions that require root canal treatment are as follows:
Pulp (the soft layer of blood vessels and nerve tissues in the innermost part of the tooth) diseases:
Irreversible pulp inflammation:
When the pulp is so severely and permanently inflamed that it can no longer heal. The inflammation is so advanced that the body's self-repair mechanisms are no longer sufficient. Even if the source of the problem is eliminated (e.g., the caries is removed), the pulp cannot heal, and the process results in complete loss of tooth vitality (necrosis).
Symptoms include:
Spontaneous pain: A throbbing pain that starts suddenly, without any trigger.
Night pain: Pain that wakes the person from sleep, especially at night. This is due to the increased blood pressure in the head area in the supine position, which further increases the inflammatory pressure in the pulp.
Prolonged pain: After being triggered by a stimulus such as cold, heat, sweet, or sour, the pain persists for several minutes (10-30 minutes or more) even if the stimulus is removed.
Pain that increases with heat and decreases with cold:In advanced cases, hot stimuli may aggravate the pain, while cold stimuli may provide temporary relief.
Radiating pain: The pain often radiates from the affected tooth to other areas (ear, temple, jawbone, or other teeth). The patient may not be able to clearly describe which tooth hurts.
Ulcerative and hyperplastic pulpitis:
Ulcerative pulpitis
A chronic form of irreversible pulpitis in which open sores form on the surface of inflamed pulp tissue. It usually occurs in teeth with a large, open carious cavity. When deep decay reaches the pulp, the pulp chamber opens to the external environment. There is a constant bacterial irritation through this opening. Pulp tissue tries to resist this chronic irritation and forms ulcers (wounds) on its surface. Root canal treatment is the definitive treatment. The pulp tissue can no longer heal and must be removed. Symptoms:
Pain: Severe pain occurs when food fills the carious cavity during chewing and presses on the ulcerated pulp tissue.
Temperature sensitivity: Hot stimuli intensify the pain.
Cold effect: Cold stimuli or cold water can relieve pain (as it reduces edema and pressure in the area).
Spontaneous pain: Pain is often triggered by eating or when something touches the tooth.
Appearance: On dental examination, a red, ulcerated tissue can be seen at the bottom of the carious cavity, which can bleed when touched.
Hyperplastic pulpitis (Pulp polyp)
This is a reaction of the nerve tissue in the tooth (pulp) to a mild and long-term irritation. As a result of this irritation, the nerve tissue grows excessively (hyperplasia) and forms a fleshy mass called a polyp into the cavity carved by the decay. This is the main reason for the appearance of what is incorrectly called "meat growing out of the gum" among the people.
This is usually seen in young teeth (deciduous molars and newly erupted permanent molars) with a strong root structure and a large, open cavity. Because the nerve tissue in young teeth is very alive and has good blood circulation, it grows excessively as it tries to heal itself and resist irritation. As a result, this growing tissue completely fills the cavity created by the decay. The canal requires root treatment. The growing pulp tissue (polyp) is removed during root canal treatment.
Symptoms:
Pain: There is usually little or no pain. This is due to the condition being chronic and progressive.
Bleeding: Polyp-shaped tissue may bleed easily when touched or chewed.
Appearance: A pink-red-colored, flesh mole-like tissue, usually with a stalk, grows out of the carious cavity. Its surface may be rough or smooth.
Temperature sensitivity: Not evident.
Pulp necrosis:
Pulp necrosis is the death of the living nerve and vascular tissue (pulp) inside the tooth. This death occurs when the tooth is suddenly cut off from the blood supply due to severe or prolonged inflammation or trauma. The tooth may change color, becoming grey or yellowish, and will not respond to stimuli such as heat or cold. The only treatment for this condition is root canal treatment, which removes dead tissue from the tooth.
Diseases of the tissue around the tooth:
Tissue Diseases Around the tooth are generally called periodontal diseases and affect the tissues surrounding and supporting the tooth (gum, bone, and ligament).
Gingivitis:
This is the mildest and most reversible first stage of the disease. It only affects the gums (gingiva).
The main cause is bacterial plaque that accumulates on the teeth. Inadequate oral hygiene allows plaque to form.
Symptoms:
- Red, swollen and shiny gums (Healthy gums are pink, firm and look like orange peel)
- Bleeding when brushing teeth or spontaneously (The most important and early symptom!)
- Bad breath
Inflammation of the gums and jawbone:
If gingivitis is left untreated, the inflammation progresses deeper into the gums and passes into the stage called periodontitis, where irreversible damage begins. At this stage, destruction of the bones and fibers holding the tooth begins.
Symptoms:
- Gingival bleeding
- Gingival recession (root surfaces are exposed, teeth appear elongated)
- Formation of deep pockets (periodontal pockets) between the teeth and gums, which should not normally be present
- Loosening of the teeth due to bone loss
- Bad taste in the mouth and persistent bad breath
Gingival recession:
It is the displacement of the gum in a way that leaves the root surface exposed. Since the root surface is opened, hot-cold sensitivity and caries risk increase.
Causes:
- Periodontitis (most common cause)
- Harsh and traumatic tooth brushing
- Teeth clenching or grinding (bruxism)
- Abnormal tooth alignment
Gingival abscess:
Inflammation (pus) accumulated in the periodontal pocket is trapped in the tissue and causes swelling.
Symptoms: Severe, throbbing pain, redness, swelling, and shaking of the tooth.
Canal filling:
This stage involves sealing the cleaned and shaped root canal system.
Filling the canal: Once healing is assured (in multi-session treatments), the canals are filled with a special filling material up to the root tip.
Sealing the canal entrance: The root canal filling is sealed to prevent reinfection of the canal system. For this, a suitable filling material is placed.
Root canal treatment usually consists of the following stages:
Clinical examination and diagnosis:
- The physician listens to what the patient wants treatment for and asks questions about their symptoms. The absence of acute pain, swelling or obvious symptoms (e.g., referred patients) is recorded at this stage. Previous treatments, traumas, and general state of health are also important.
- The dentist assesses the appearance, texture and color of the intraoral and extraoral tissues and the presence of fistulas. The restoration status of the tooth, the presence of caries, fractures, and periodontal support are also examined.
- The vitality of the pulp is assessed by thermal tests (cold/hot) and electric pulp testing (EPT). In the case of irreversible pulpitis, pain persists even after the stimulus is removed. The cold test is effective for vital teeth. A reference point is established using control teeth.
- Conventional periapical radiographs and, if necessary, cone beam computed tomography (CBCT) are used to assess the anatomy of the tooth, pulp chamber, canal morphology, root resorption, and periapical pathologies.
- By combining all this information, a definitive diagnosis is made about the condition of the pulp and periapical tissues.
Preparation:
This stage involves mechanical cleaning and shaping of the root canal system.
Anesthesia: The treatment starts with local anesthesia to make it painless.
Isolation: The tooth to be treated is isolated with a rubber sheet to protect it from saliva and other microorganisms, as well as to prevent the patient from swallowing the instruments or chemicals used.
Root canal treatment:
Caries cleaning and pulp removal: Existing caries is completely cleaned, and inflamed or damaged pulp tissue is removed.
Access to the pulp chamber: An access cavity is made through the crown of the tooth into the pulp chamber. This cavity is enlarged to provide straight access to the root canal system. The color of the pulp chamber floor (darker than the canal walls) helps to determine the location of the canal orifices.
Determination of Working Length: The length to the root tip, where the canal will be cleaned and shaped, is precisely determined using an electronic apex locator and radiographs.
Shaping of root canals (instrumentation): The original shape and apical stenosis of the canal are preserved, and a tapering conical shape is given from the corona to the apex. The crown-down technique is generally preferred. Stainless steel hand instruments (K-type, Hedstrom files) and nickel-titanium (NiTi) rotary instruments are used for this procedure. NiTi instruments offer advantages such as flexibility and resistance to fatigue.
Channel washing: In addition to mechanical cleaning of the canals, copious flushing is performed using antibacterial and tissue-dissolving solutions such as sodium hypochlorite (NaOCl).Irrigation provides disinfection of areas inaccessible to instruments.
After the treatment is completed, there are some points that the patient should pay attention to:
Pain and sensitivity: After the treatment, mild pain and sensitivity may be felt in the tooth for a few days. In this case, painkillers can be used. In case of severe or persistent pain and swelling, a physician should be consulted.
Tooth fragility: Teeth that have undergone root canal treatment may become more fragile due to pulp loss and loss of material. For this reason, it is recommended not to chew very hard foods.
Permanent filling/coating: After taking measures to prevent re-decay and infection of the treated tooth, permanent filling or coating may be required to ensure the durability and aesthetics of the tooth.
Check-ups: Regular dentist control is essential for the lifelong use of a root canal-treated tooth.
The main benefits of root canal treatment are as follows:
Natural Tooth Recovery: The most important benefit is that it saves an inflamed or damaged tooth from extraction. In this way, the patient's own natural tooth remains in the mouth.
Elimination of pain: It relieves severe, spontaneous, and prolonged pain experienced in conditions such as irreversible pulp inflammation. Since local anesthesia is applied during the treatment, pain is usually not felt.
Prevention and treatment of infection: It prevents the spread of infection to surrounding tissues and treats existing infections by removing inflamed or necrotic (dead) pulp tissue and microorganisms from the canals.
Long-lasting use: When appropriate restorations are made after treatment and regular oral hygiene and dentist controls are provided, a root canal-treated tooth can be used for a lifetime.
Preservation of chewing function: Retaining the natural tooth in the mouth helps to maintain correct chewing function, continuity of the dental arch, and the vertical dimension of the face.
Maintaining aesthetics: The aesthetic appearance of the tooth is restored with a permanent filling or crown on the treated tooth.
Preventing jawbone loss: By preventing tooth extraction, it prevents jawbone loss and shifts in neighboring teeth that may occur after extraction.
Supporting root development in immature teeth: In teeth with incomplete root development (immature), it ensures the continuation of root tip development in cases where the living pulp can be preserved.
Creating a basis for restoration: It enables a tooth that is damaged or has lost material to form a solid foundation for permanent restorations such as crowns.
Although root canal treatment is a successful treatment option for many patients, in some cases it may not be suitable or may significantly reduce the chances of success. Here are the conditions that may not be suitable for root canal treatment:
- If the bone tissue surrounding the tooth is severely eroded or the tooth is excessively shaking due to periodontal disease, it may not be possible to save the tooth.
- If there are vertical or deep cracks in the roots, the risk of recurrence of infection is high. Root canal treatment cannot repair these fractures. Teeth with broken roots are usually extracted.
- If the crown (upper) part of the tooth has lost too much material due to decay or fracture and cannot be restored with filling/capping, root canal treatment may be meaningless.
- The root canals of some teeth are extremely narrow, calcified, or have complex anatomy. In these cases, the canals cannot be fully cleaned and filled. Treatment may fail; the tooth may be extracted.
- The risk of infection is high in patients with uncontrolled diabetes, patients receiving chemotherapy, immunocompromised individuals, or those with heart valve prostheses. These conditions may not be an absolute obstacle, but the physician should evaluate the general health status before treatment.
- Root canal treatment may take more than one session, and if the patient is unable to attend regular check-ups or maintain oral hygiene, the treatment may fail.
Is root canal treatment a painful procedure?
No. Thanks to modern anesthesia techniques, no pain is felt during the procedure. The slight sensitivity that may occur after the procedure is easily controlled with painkillers.
How long does root canal treatment take?
It depends on the condition of the tooth. It is usually completed in 1-3 sessions. Each session can last approximately 60-90 minutes.
Is there pain after root canal treatment?
A slight tenderness and swelling for a few days after treatment is normal. This can be managed with painkillers and cold compresses recommended by the physician.
Will the treated tooth decay again?
Yes. The upper part of the tooth (crown) can still decay. Therefore, it is very important to pay attention to oral hygiene and go for regular check-ups.
Can root canal treatment fail?
Yes, in rare cases it can. Reasons may include incomplete cleaning of the canals, hidden canal exits, or the crown restoration not being sealed. In case of failure, the treatment may be repeated, or surgical intervention (apicectomy) may be necessary.
Will my tooth break after treatment?
Yes, teeth that have undergone root canal treatment can be more fragile. For this reason, doctors usually recommend a crown over the tooth. This protects the tooth and reduces the risk of fracture.
Can every tooth have root canal treatment?
A: No. If there is too much loss of bone surrounding the tooth, if there is an irreparable crack in the roots, or if the tooth is too damaged to be restored, it may be necessary to extract the tooth.
How to choose between root canal treatment and an implant?
Preserving the natural tooth is always the better option. Root canal treatment is usually less costly and less invasive than an implant. However, if the tooth cannot be saved, an implant is the best alternative.
Does root canal treatment affect general health?
It contributes positively to general health by eliminating the source of infection in the mouth. Untreated dental infections can negatively affect other parts of the body (heart, kidneys).
What should I do if a temporary filling falls out?
You should contact your dentist as soon as possible. If the temporary filling falls out, it may cause the canals to become infected again.
Is it necessary to use antibiotics before root canal treatment?
Your dentist may prescribe antibiotics only if there is an active and widespread infection (swelling, fever). It is not a routine practice.
Is root canal treatment also performed in children?
Yes, "pedodontic root canal treatment" (pulpotomy/pulpectomy) can be applied to deciduous teeth. This is important for the underlying permanent tooth to remain healthy and serve as a placeholder.
Does tooth color change with root canal treatment?
Rarely, treated teeth may turn grey over time. In this case, aesthetic treatments such as internal bleaching or porcelain veneers can be applied.
How long is the life span of a tooth with root canal treatment?
If a good root canal treatment and a good restoration (filling/capping) are performed, the tooth can remain in the mouth for a lifetime.
Does the tooth lose sensation after root canal treatment?
Yes, since the nerve tissue inside the tooth is removed, the tooth no longer feels stimuli such as hot/cold. However, since the tooth is connected to the jawbone, it continues to feel the chewing pressure. This loss of sensation means that the tooth has lost its vitality, but the tooth continues to function.
Can root canal treatment and teeth whitening be performed at the same time?
No, whitening can be considered after the root canal treatment is completed and the tooth has healed. The priority is to save the tooth from infection and restore it. Your dentist will determine the appropriate time for whitening.
Does the infection recur after root canal treatment?
In rare cases, it may recur. The main reasons for this are the presence of narrow / complex canals that are difficult to clean, the crown filling is not sealed, or a new trauma. If the infection recurs, renewed treatment or surgical intervention (apicectomy) may be necessary.